Key Takeaways:
- Gout can be hereditary. Genetics can affect how the body handles uric acid, increasing the risk of developing the condition.
- Flares are just one phase. Even when symptoms disappear, crystals may continue to build, so ongoing management is important.
- Early action can slow progression. Without treatment, gout can worsen over time and lead to joint damage.
- Lifestyle still influences risk. Diet, weight, hydration, and overall health play a key role alongside genetics.
- Proactive care makes a difference. Timely treatment and research-supported approaches.
Most people think gout is simply caused by eating rich food or drinking alcohol, but that’s not the full story. The truth is that genetics plays a much bigger role than many people realize. Gout happens when uric acid builds up in your blood and forms tiny, sharp crystals in your joints. That’s what causes sudden, intense pain and swelling, often in the big toe. Normally, your body flushes uric acid through urine. But if you’ve inherited certain genetic traits, your body may not remove them efficiently, increasing your risk of painful flare-ups. In fact, a major study involving 2.6 million people identified hundreds of genetic links to gout. So, if it runs in your family, it may be more than just a lifestyle; it could be in your DNA.
In this blog, we’ll break down how genetics influences gout, what the local clinical research programs reveal, and what you can do to lower your risk and better manage the condition.
Is Gout Hereditary? Understanding the Genetic Link
Research shows that genetics account for a significant portion of gout risk. In fact, studies estimate that the heritability of gout may be as high as 60–65%. That means your DNA can strongly influence whether you develop the condition. Gout develops when uric acid builds up in the bloodstream. Uric acid forms when your body breaks down purines, natural compounds found in your cells, and in certain foods like red meat and seafood. Normally, your kidneys filter uric acid through urine. But when that system doesn’t work efficiently, uric acid levels rise; crystals form in the joints, and inflammation begins.
Certain genes, like SLC2A9 and ABCG2, control how uric acid is transported and excreted from your body. If you inherit variations in these genes, your body may absorb too much uric acid or fail to eliminate enough of it. Over time, that increases your risk of hyperuricemia (high uric acid), which can lead to gout. About 1 in 5 people with gout have a close relative who also has the condition. If a parent or sibling has gout, your chances increase, but your lifestyle still plays a major role.
What Happens During an Acute Gout Flare?
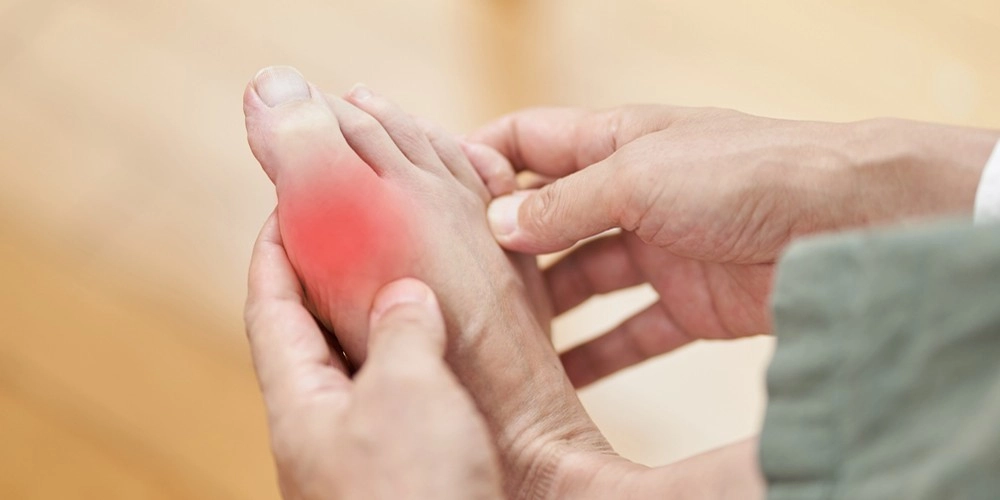
When most people think of gout, they picture the flare, and for good reason. An acute gout attack is sudden, intense, and often strikes without warning, commonly in the middle of the night. The big toe is the classic target, but gout doesn’t stop there. It can also affect the ankle, knee, wrist, or even your fingers. During a flare, the affected joint may become:
- Noticeably swollen
- Bright red
- Warm to the touch
- Extremely tender
- So sensitive that even a bedsheet brushing against it feels unbearable
However, this pain can be severe enough to disrupt sleep, limit walking, and interfere with daily life. Moreover, there are some common triggers including, alcohol (especially beer), high-purine foods like red meat and shellfish, dehydration, sudden illness, stress, or certain medications. If your first flare occurs at a younger age, you might wonder if gout is hereditary, especially with a family history. Your risk is also determined by when flares begin and how severe they become.
Understanding Intercritical Gout
After the flare settles, you enter what’s known as the intercritical gout, the quiet period between attacks. During this time, everything may feel completely normal. No swelling. No redness. No pain. But don’t be fooled. Even when symptoms disappear, uric acid crystals can continue forming silently inside the joints. This is what makes intercritical gout tricky. Many people assume the problem has been resolved when, in reality, the underlying imbalance remains. However, these genetic factors can affect how frequently flares return. Some people go years between attacks. Others experience them more regularly. That’s why managing uric acid levels, even when you feel fine, is essential to prevent future flares and long-term joint damage.
How the Disease Progresses Over Time
Gout rarely begins with permanent joint damage or visible deformities. In fact, it often develops slowly and quietly before the first painful attack ever happens. The stages of gout unfold gradually, and understanding how the disease progresses over time can make a significant difference in preventing long-term complications.
Recognizing the early signs, even before symptoms appear, allows individuals to take steps that may reduce flares, protect joints, and slow progression. Here are the four main stages of gout explained in a clear and practical way:
1. Asymptomatic Hyperuricemia
This early stage occurs when uric acid levels in the blood are elevated, but there are no noticeable symptoms. Many people live for years in this phase without realizing their uric acid levels are high because there is no pain or swelling to signal a problem.
Although it may seem harmless, uric acid crystals can begin forming silently in the joints during this time. Not everyone with high uric acid will develop gout, but this stage sets out the foundation for future flare-ups if levels remain uncontrolled.
2. Acute Gout Flare
This is often the first clear sign that something is wrong. An acute gout flare usually appears suddenly, often at night, with intense joint pain, swelling, redness, and warmth. The big toe is commonly affected, but other joints such as the ankle, knee, or wrist can also be involved.
The pain can feel sharp, throbbing, or unbearable; even the weight of a bed sheet may feel uncomfortable. These flares can last several days to a week or more, especially without treatment.
3. Intercritical Gout
After a flare subsides, the body enters what is known as intercritical gout, the symptom-free period between attacks. The joint may feel completely normal again, which can make it tempting to ignore the condition.
However, beneath the surface, uric acid crystals may continue to accumulate. Without management, future flares can become more frequent, last longer, and affect additional joints over time.
4. Chronic Tophaceous Gout
If gout remains untreated or poorly managed for years, it can progress into chronic tophaceous gout. At this stage, repeated inflammation can lead to ongoing joint pain and stiffness.
Hard deposits of uric acid crystals called tophi may form under the skin, commonly around the fingers, toes, elbows, or ears. These deposits can cause visible swelling, joint deformity, and in severe cases, permanent joint damage or reduced mobility.
Furthermore, understanding how gout progresses empowers people to act earlier. While genetics may influence who develops gout and how quickly it advances, early diagnosis, lifestyle adjustments, and appropriate treatment can significantly slow, and sometimes prevent, progression to the more advanced stages.
Risk Factors Beyond Genetics
While genetics absolutely plays a main role, many people ask, “Is gout hereditary?” As it’s only one piece of the puzzle. Your daily habits, overall health, and metabolic conditions can significantly influence whether gout develops and how severe it becomes.
Several non-genetic risk factors can increase uric acid levels or make flare-ups more likely, including:
- Obesity, especially excess abdominal fat
- High blood pressure
- Diabetes and insulin resistance
- Kidney disease
- Regular alcohol consumption
- A diet high in purines (such as red meat and shellfish)
- Certain medications, particularly diuretics (water pills)
Abdominal fat is particularly important because it releases inflammatory chemicals that can intensify gout attacks. Alcohol, especially beer, can interfere with how the liver processes uric acid, leading to higher levels in the bloodstream. Meanwhile, if kidney function is reduced, the body struggles to eliminate uric acid effectively, leading to its accumulation and the formation of crystals in the joints.
Diagnosis and Treatment
If you suspect gout, a healthcare provider may use:
- Blood tests to check uric acid levels
- Joint fluid analysis to detect urate crystals
- Imaging tests like ultrasound
Treatment focuses on two goals:
- Relieving pain during acute flares
- Lowering your uric acid levels long-term
Medications like allopurinol or febuxostat help reduce uric acid production. Anti-inflammatory drugs help manage flare pain. If you have a family history and still wonder, is gout hereditary? Talking to a healthcare provider early can help you monitor uric acid levels and prevent further complications.
Research and Clinical Opportunities
For individuals living in Alexandria, there are ongoing opportunities to participate in clinical research related to gout and other rheumatologic conditions. Local programs, such as rheumatology studies near Alexandria, provide information on ongoing research into inflammatory joint conditions. Individuals experiencing active attacks may qualify for gout flare clinical trials in Alexandria, where new treatment approaches are being evaluated. Broader opportunities are available through Alexandria Clinical Trial Programs, which include studies across multiple therapeutic areas. For individuals concerned about hereditary risk, research participation may also help improve understanding of how genetics influences gout.
Acute Gout Flare Clinical Trials
Explore active clinical trials for fast relief from acute gout flare pain
Final Thoughts
Genetics can increase susceptibility, particularly through inherited differences in how the body regulates uric acid. However, family history does not mean the condition is unavoidable. But understanding your risk, recognizing early symptoms of a gout flare, and managing the condition proactively can make a meaningful difference. Also, taking simple lifestyle measures, such as monitoring uric acid levels, maintaining a healthy weight, staying well hydrated, limiting alcohol intake, and seeking timely medical advice, can help reduce flare frequency and protect joint health.
Even with a genetic predisposition, informed choices and early care can support better long-term outcomes and a higher quality of life. If you’re considering more advanced care pathways, exploring clinical trial opportunities focused on gout and related rheumatologic conditions may be beneficial. For dependable research, expert-led perspectives, and guidance grounded in evidence-based care, connect with Northshore Research Associates, your partner in improving outcomes for gout and arthritis management.



